A last resort against COVID-19
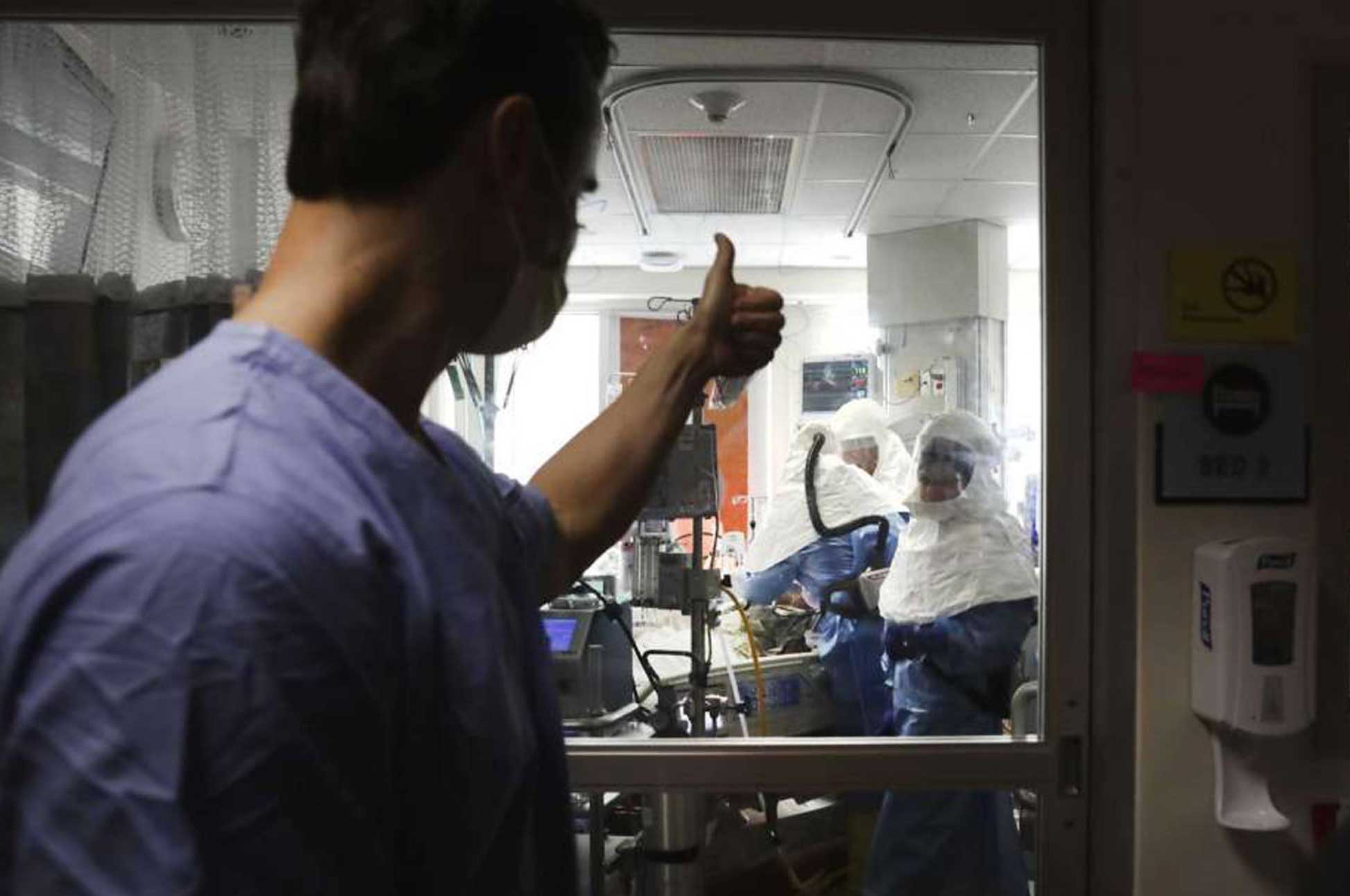
Photo Details: Dr. Jeff DellaVolpe gives a thumbs up to doctors and nurses performing an intubation on a coronavirus patient at Methodist Hospital, which is using ECMO to help add oxygen to patients’ blood. (Bob Owen, San Antonio Express-News | Express News)
Dora Wilson had just brought her husband home from the hospital, oxygen tank in tow, when their son appeared at the back door, looking ill.
Paul, a 71-year-old military veteran, had spent nearly two weeks at Brooke Army Medical Center with COVID-19. Dora, 68, also tested positive for the coronavirus and felt miserable, but she was well enough to remain at home with Nick, their son.
Although Nick had developed a fever and other symptoms, Dora hadn’t heard much complaint from him while he cooked for her and left the meals at her bedroom door, even as her appetite vanished.
But now Nick was telling her that he needed to go to an emergency room.
“I can’t breathe,” he said.
At 30, with no serious health problems, Nick seemed in the best position of any of them to fight off the virus.
Instead, he would become the sickest of them all.
Over the next few days, as Nick’s breathing deteriorated and his oxygen levels plummeted, he would be treated at four hospitals in San Antonio as doctors sought to save his life.
His case would illustrate the lengths to which health care workers have to go to fight an aggressive viral pneumonia that has proved an unpredictable, formidable opponent.
It would also become a testament to the challenges and limitations they face.
With no proven treatments for COVID-19, medical teams have been left to improvise. They have turned to oxygen and ventilators, to experimental drugs and therapies. What works for one patient won’t necessarily work for another.
In Nick’s case, when even medications and a ventilator weren’t enough, he was given extracorporeal membrane oxygenation, or ECMO, which allowed his lungs to rest as a machine took over the job of filtering oxygen into his blood. Such devices are even scarcer than ventilators, and they’re more invasive, coming with their own risk of complications.
But other options had been exhausted. It was his best chance of survival.
The virus came first for Nick’s father.
When Paul, a ride-share driver, began feeling ill in March, he went to BAMC’s emergency department, where he was given antibiotics and a test for COVID-19. The results came back positive March 23.
Within two days, his breathing worsened, and he was back in the hospital. This time, he was transported there by emergency responders in protective gear.
It came next for Dora.
While Paul was in the hospital, the semi-retired speech pathologist was at their Northwest Side home with Nick, who had been laid off from his job at a car wash after the pandemic hit. Dora developed a fever, fatigue, diarrhea and a headache so severe it woke her up in the middle of the night.
The two kept to separate areas of the house. When they were about to enter common areas like the kitchen, they would call out to each other as a warning.
But in the end, it came for Nick, too.
He was hit by fever, chills and diarrhea in late March. Still, he could fetch meals and fluids on his own.
About that time, his father was transferred to the intensive care unit. But so far, he hadn’t needed a ventilator.
On April 6, a day after Dora’s symptoms resolved, Paul was ready to be released from the hospital. Dora picked him up and drove him home. As they got out of the car, she could see how ill her typically happy, upbeat son looked. She was shocked since he hadn’t complained about, or even mentioned, how badly he was feeling.
Nick was, too. He knew he was infected, but he thought he’d be back on his feet after a week or two in bed. The breathing problems developed so quickly that it caught him by surprise. Suddenly, walking 5 feet to the bathroom left him winded.
As he told his mother he needed medical care, she could hear him pausing to catch his breath before he spoke.
She watched as one sick family member replaced the other in the car.
Dora drove Nick to the nearest hospital, a freestanding emergency room in the Baptist system.
The doctors admitted him. By phone, one told Dora that her son wasn’t doing well and needed supplemental oxygen.
Over the next few days, the calls grew more alarming.
On April 9, Dora learned that Nick was receiving the maximum amount of supplemental oxygen, and his fever was nearing 103 degrees. He needed to be transferred to a facility where he could be put on a ventilator, if it came to that.
Dora began to despair.
Nick was taken across town to Northeast Baptist Hospital, where the hospital system had centralized care for its critical COVID-19 patients.
When Dr. Tamara Simpson, a critical care pulmonologist, met Nick in the ICU, she was struck by how young and frightened he looked. On top of that, she learned he had fallen ill while taking care of his parents.
The conventional wisdom is that the coronavirus poses the most risk to the elderly and those with chronic health problems. But that wasn’t Nick, she thought. He had a history of mild asthma and high blood pressure — nothing serious enough to justify his dire state.
Why was it that his parents were recovering, but their young, previously healthy son was doing so poorly?
To Simpson, it was inexplicable. If this could happen to a guy like Nick, it could happen to her, to her colleagues.
Already, Simpson felt stretched thin, and she worried what that meant for her own immunity against the horrible disease she was exposed to on a daily basis.
The work of caring for these patients had proved physically and emotionally taxing. The days were long, stressful and, at times, overwhelming. With limited understanding of the virus, hospital workers had to be flexible, learning along the way.
Despite their best efforts, the outcomes weren’t always positive. On one particularly bad day, the unit’s staff broke down in tears. It felt like all their patients were dying.
With physical distancing measures in place, doctors, nurses and respiratory therapists at Northeast Baptist had to take on a more intimate role in the lives of patients and family members who were isolated from each other.
Doctors were regularly calling and texting with spouses and relatives who had no other way to get information about their loved ones. Nurses were holding the hands of patients as they died so they wouldn’t be alone at the end.
In the rare instances that family members did come to the hospital to see a dying patient, conversations that normally were private had to be facilitated by medical workers. In those cases, the patient would be rolled to a glass door, their loved one on the other side. Hospital staff would hold up two-way radios so they could communicate.
“They are saying what they want to tell their loved ones, where we can all hear it. And there’s not a dry eye in the ICU,” Simpson said. “You just see the love, and the hurt.”
Simpson didn’t want that to happen to Nick.
The week that Nick arrived at Northeast Baptist was a particularly busy one for the hospital. At one point, 18 COVID-19 patients were simultaneously on ventilators — the most of any hospital in the city.
Nick would soon be among them.
On an X-ray, the lungs of a healthy person appear black. Images of Nick’s lungs had shown an accumulation of “ground glass” — hazy, white patches that were evidence of spreading inflammation in the delicate tissue.
Simpson knew things were not looking good for him. He was on antibiotics and hydroxychloroquine, a controversial anti-malaria drug being used to treat some COVID-19 patients. His oxygen levels were low. A ventilator was the next step.
Before sedating and intubating him, Simpson told Nick he could briefly talk with one family member. She reminded him to sign off with “see you later,” rather than “goodbye.”
He chose his mother. On the phone, he told her he was scared.
Sick with worry, Nick’s parents drove to the hospital. They waited in the parking lot until they had confirmation that the procedure had gone smoothly.
It had. But Simpson hoped she could do more for him.
Simpson knew Methodist Hospital was the only place in San Antonio treating COVID-19 patients with ECMO, which replaces the function of the lungs, and in some cases the heart too, for patients with a high chance of dying.
Initially used only with pediatric patients, ECMO had increasingly become a method of last resort for drowning victims, people with pneumonia, those suffering from heart attacks — and for a small number of COVID-19 patients.
Simpson began talking with the doctors in Methodist’s program, making her case for Nick to be accepted as a patient.
Weeks earlier, when the Methodist system had begun planning for the coronavirus pandemic, the ECMO staff was unsure whether the machine could be used to treat COVID-19 patients. Much was unknown about the novel coronavirus and the virulent respiratory illness it could cause.
If the hospital had too many coronavirus patients, ECMO might not be feasible. It demands the attention of many specialists: lung, heart, kidney, perfusion, infectious disease.
There were ethical considerations, too.
The procedure can lead to serious complications, including bleeding, infection, damaged blood vessels, the formation of clots and kidney damage. For patients considered for ECMO, the benefits have to outweigh those risks. It’s also offered at few hospitals, so it would not be available to every patient.
Still, Methodist had more capacity and expertise than most hospitals. In the past few years, it had rapidly grown into a high-volume ECMO center, treating nearly 150 patients the previous year, compared with just 27 two years before that. And the devices had played a major role during the 2009 H1N1 flu pandemic.
The ECMO team drew up plans for infection control and the admission of multiple patients at a time. They scrounged up a few extra machines. And they formed a committee to assess patients for whom nothing else had worked. They decided the procedure would be reserved for younger people without other health issues — those who stood the greatest chance of benefiting.
As coronavirus hospitalizations began to tick up in San Antonio, evidence began to emerge that ventilators were not the answer for some of the sickest coronavirus patients. Many ventilated patients were still not getting enough oxygen. They were dying.
A ventilator works by mechanically forcing air into the lungs, which are not accustomed to such pressure.
Patients can usually tolerate some amount of this, but over time, ventilation can stretch and damage small tissues in the lungs. And in some patients with respiratory failure, including a subset of those with COVID-19, it doesn’t matter how much oxygen is forced in. The lungs can be so damaged that the oxygen does not make its way to the rest of the body, to the cells and tissues that need it.
With ECMO, the lungs are removed from the equation. Large tubes are fed into arteries and veins so a machine can remove blood from the body and oxygenate it directly before returning it. Under the right conditions, it allows doctors to hit the pause button, giving a patient’s organs time to rest and recover.
After Nick’s intubation, Simpson called Dora and told her she was considering him for other treatments. She had ECMO in mind, but she was intentionally vague, careful not to raise Dora’s hopes in the event that he wasn’t accepted by Methodist as a patient.
She was relieved when the hospital agreed to take him.
In the meantime, Dora wanted to see her son. So Simpson donned protective gear and, with her cellphone in a bag, placed a video call to Dora and held the phone in front of Nick. The doctor encouraged Dora to talk to Nick, who was still under sedation, sure that he would be able to hear her.
Dora relayed every encouragement she could think of. He was strong, he could fight this, he was going to be fine.
They were counting on him to pull through.
The following day, Easter Sunday, things took a turn. Nick hadn’t taken well to the ventilator. He was getting worse by the hour.
Over the phone, Simpson explained ECMO to Dora and got her permission to transfer Nick to Methodist’s care. He arrived at the hospital later that day.
Like Simpson, Dr. Jeff DellaVolpe, co-medical director of Methodist’s ECMO program, was struck by how young Nick was, and how ill. He was receiving close to 100 percent oxygen from the ventilator, yet that was not improving his oxygen levels. He wanted to give someone like him, someone sickened while caring for his family, a fighting chance.
DellaVolpe knew the coronavirus behaved differently than other respiratory viruses. Usually, viruses would interfere with the delivery of oxygen by causing a person’s lungs to grow stiff, making them hard to inflate with a ventilator.
That wasn’t happening with this virus. The lungs of these patients still were flexible, yet they had dangerously low oxygen levels. The reasons were not yet known, but it was clear to DellaVolpe that medicine’s traditional assumptions might not apply to these patients. Maybe ECMO could help.
It had been less than a week since Methodist had begun treating COVID-19 patients with ECMO. Nick would be among the first.
That evening, as DellaVolpe was preparing to hook Nick to the ECMO machine, he called Dora. He asked about her son’s medical history and whether she understood how rapidly he was deteriorating.
Then he went to work.
For hours, Dora didn’t hear anything. Then, in the middle of the night, her phone pinged with a text.
It was from Nick.
Worried that it was a prank, some horrible joke, she called the nurses’ station.
“Oh yeah, he’s awake,” the nurse said. They had just extubated him, so she wasn’t sure if he could talk yet.
Dora wrote back: “Oh my son!!! Please get better! Keep being strong & fighting this disease!”
Then, Nick said, “BTW, I could hear you earlier.” He was referring to Dora’s conversation with him while he was sedated.
When Dora sent Simpson a screenshot of the exchange, she couldn’t believe it.
Over the next few days, Nick steadily improved.
Some patients can remain on ECMO for weeks or even months, but he was weaned from the machine after only three days. He needed supplemental oxygen, but he was breathing on his own, a major step forward. He was moved to Methodist Ambulatory Surgery Hospital, where many of the system’s coronavirus patients were being treated.
Nick is among a tiny subset of coronavirus patients to have been treated with ECMO. According to a registry created by the Extracorporeal Life Support Organization, which tracks data from ECMO centers around the world, hospitals reported its use on more than 500 COVID-19 patients, including nearly 400 in North America.
Simpson is thrilled by Nick’s recovery and the collaboration that led to it. She has sent a handful of her patients to Methodist, which has treated about a dozen coronavirus patients with ECMO. She now touches base with the team daily.
In her conversations with DellaVolpe, she pre-emptively advocated for herself — if she gets sick, she told him, she would want the same medical care Nick received.
She feels “forever connected” to the Wilson family. It was heartening to be involved in a successful case, to see a COVID-19 patient in such a severe condition make it through.
Her experiences treating him and other coronavirus patients have solidified her belief that it is too soon to ease lockdown restrictions. She has never seen a disease strike multiple members of the same family the way COVID-19 has.
For DellaVolpe, cases like Nick’s illustrate the gravity with which the coronavirus should be taken.
“I’ve been struck by how many young, previously completely healthy patients really are to the point where they almost die. It’s a scary thing,” he said. “It’s something that we should be aware of and have respect for.”
On Wednesday evening, Nick was discharged from the hospital and wheeled out of the ambulance entrance. He was wearing the same protective equipment as the medical personnel accompanying him — gloves, a gown, a mask and a face shield.
His mother was so happy, she could not stop crying.
Nick and his family are grateful, to the health care workers who cared for him, and for the friends and family who kept him in their prayers.
By text, he said he is “ecstatic” to be back home with a “mostly” clean bill of health.
He has an arduous recovery ahead. He remains weak and has trouble walking, standing and sitting. His body is covered in wounds from IV lines and the enormous ECMO tubes. His family will keep a close eye on him for signs of regression or blood clots, a serious complication in some COVID-19 patients.
After everything he has been through, he feels it is too soon for daily life to return to what it was.
“I may have gotten past this, but people need to understand that I was on death’s doorstep several times, and it’s only through the grace of God that I survived. I got lucky,” Nick said.
“Most people won’t.”
About ECMO
Patients with severe cardiac and respiratory failure now have an option for air transport on ECMO with a specially trained ECMO team and mobile ECMO unit.
ECMO Transport boasts an experienced team working directly with you, your institution and the receiving facility to safely transport your ECMO patient. We can safely transport patients domestically or even internationally.
In collaboration with our CAMTS-accredited air carrier, ECMO Transport offers fixed-wing transport for any ECMO patient. Our transport services are available 24 hours a day, 7 days a week, 365 days a year. We are unique in that we staff an ECMO-trained physician on board, as well as an ECMO specialist and the equipment necessary for carrying out the transport.
We work with the air carriers to identify facilities that can place your ECMO patient. All it takes is one call to mobilize our team, ensuring the fastest response time to transport your ECMO patient safely and efficiently.eam and mobile ECMO unit.
